In November 2023, Churchill County contracted with Winged Wolf Innovations to complete the required Opioid Misuse Needs Assessment, which is necessary to be eligible for further Opioid Settlement Funds.
In 2021, Nevada established NRS 433.712-433.744 to address the state’s portion of opioid litigation recoveries. As a result, Churchill County, along with all other Nevada counties receiving settlement funds from litigation concerning the manufacturing, distribution, sale, or marketing of opioids, must conduct an Opioid Misuse Needs Assessment and submit the findings to the state, which will be included in the Fund a Resilient Nevada Statewide Plan.
Winged Wolf Innovations is a consulting firm that provides Administrative and General Management Consulting Services, offering solutions in Organization and Leadership Development, Systems Planning and Design, Strategic Planning, and Program Development.
Churchill County Social Services Director Shannon Ernest presented key findings from the assessment to the Board of Commissioners during their May 2 meeting.
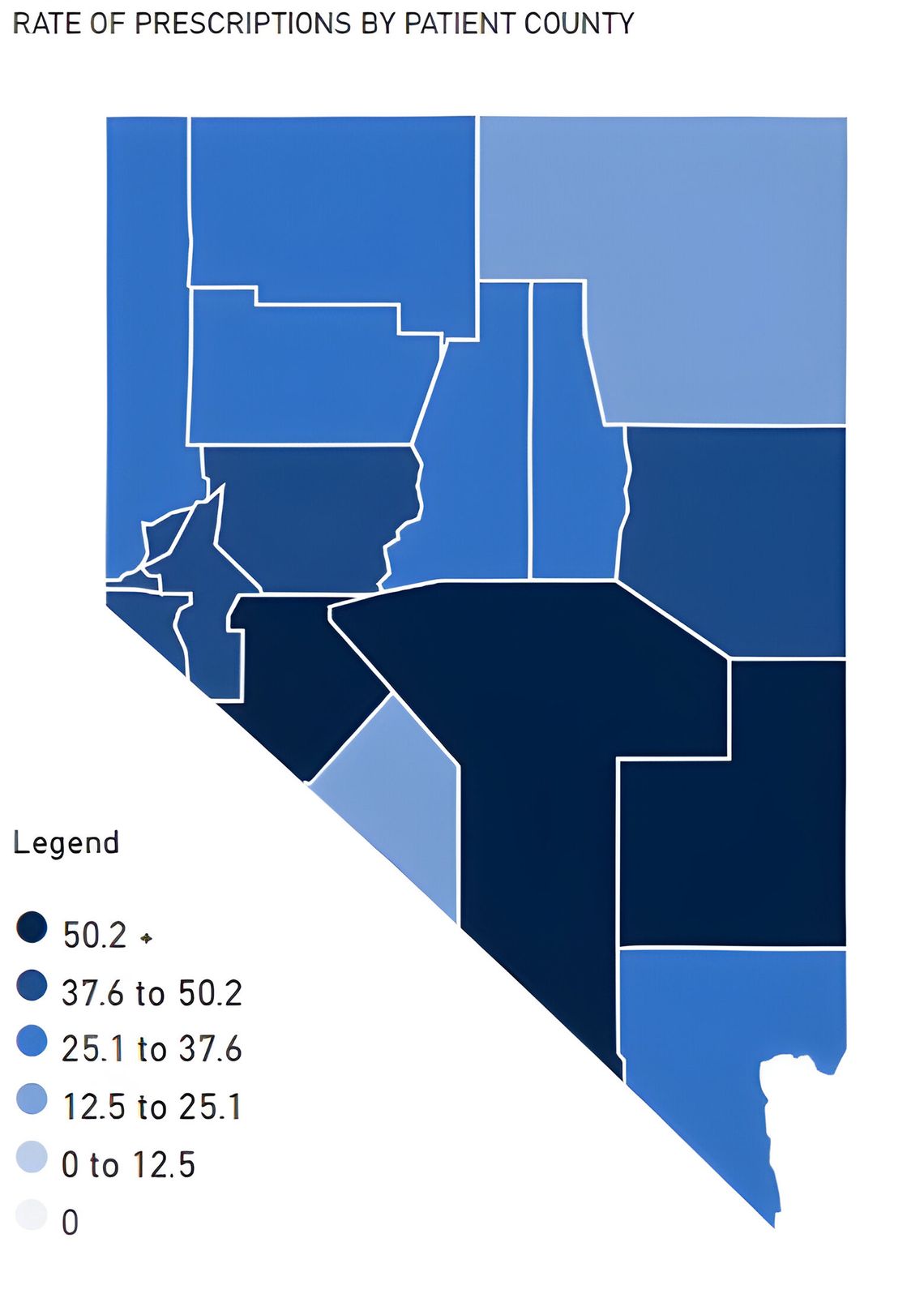
General Opioid Use: The majority of Churchill County’s opioid use was prescribed by physicians for pain management. Local prescription rates have been declining since 2017. However, they are still significant, especially compared to methadone and buprenorphine, a synthetic opioid developed in the late 1960s used to treat pain and opioid use disorders.
Dependency: White women appear to have the highest rate of opioid dependence, according to Banner Churchill Community Hospital data. Individuals who suffer from opioid dependence have significantly higher hospitalization rates than emergency department visits. However, overall inpatient visits for opioid dependency have been decreasing in the county. The Northern Nevada Behavioral Health Region (NNBHR), which includes Churchill County, has also seen a decrease in emergency visits since 2016. It should be noted that the region had the highest rate of inpatient visits for opioid dependency in Nevada from 2015 to 2020.
Overdoses: Last year, Churchill County had markedly higher suspected drug-related overdoses compared to the overall state average. Opioids are the highest contributor to substance-related deaths in the northern region. Overdoses, also referred to as “poisonings,” have been consistently higher than other substances in both emergency rooms and inpatient visits. Men, particularly young white men, are more likely to suffer opioid poisoning in Churchill County; however, the northern region has an overall lower rate of inpatient visits for opioid poisoning in the state. Suspected drug overdoses in Churchill County exceed the state average.
Crime: The number of overdoses and crimes encountered in Churchill County has been rising. There is a need for improved surveillance, particularly in reporting, identifying risk factors, increasing naloxone availability, and creating a suspected street overdose response team.
There is limited engagement between law enforcement and the community regarding the opioid crisis, primarily due to a lack of resources for extensive community education. Arrests have been made for possessing and selling opioids; however, law enforcement faces many challenges in tracking specific data, such as opioid withdrawals in jails and the number of respondents obtaining high-dose prescriptions.
Deaths: Opioid-related deaths in Churchill County have remained relatively stable, but there was an anomalous spike in 2017. Opioids are the highest contributor to substance-related deaths in the Northern Behavioral Health Region.
Medication-Assisted Treatment (MAT): Assessment participants expressed feelings of humiliation, stigma, and fear associated with seeking treatment for opioid addiction. MAT’s stringent regulations and limited awareness of its effectiveness were listed as some of the barriers to securing treatment from providers. Despite this, 50% of participants agreed that MAT is very effective.
According to the assessment, there is a split opinion within the community regarding the critical nature of opioid use and misuse. Client focus groups unanimously agreed that opioid use results from mental illness and childhood trauma, with survey respondents, including providers, supporting this view. Respondents experienced several adverse effects of opioid use, including a decline in overall mental and physical health, legal concerns, strained relationships, and other challenging issues.
Despite the consequences, opioid use continues to cause far-reaching and damaging outcomes for both users and the community. Part II will be available in next week’s edition of The Fallon Post and will include insights on student heroin use, drug diversion programs, restorative justice, and overall recommendations.













































Comment
Comments